Popping the pill: unpacking the most popular hormonal contraceptive
In the rooms of many people assigned female at birth (AFAB) across the country sits a small case full of little white and tan pills stuffed into cardboard sleeves or ugly plastic cases. The boxes they come in have fancy names like Yasmin or Aviane and neatly folded instruction manuals. They’re prescribed for a multitude of reasons ranging from acne to anemia to sexual intercourse. Oral contraception, more commonly known as the pill, is the most popular form of reversible birth control in the United States. 65 percent of AFAB people in the United States ages 15-49 use contraceptives, about 14 percent of those people choose the pill as their method according to a study conducted by The National Center for Health Statistics (NCHS) in 2018.
Despite its normalization as a remedy for teen hormonal issues (acne, cramps etc) and widespread contraceptive use, the conversation around the pill and how it works is almost nonexistent. Although the topic of contraception is covered in sophomore Urban health classes and students are asked to research them, it isn’t a long unit. “It’s a small part of our curriculum,” said Jenn Epstein, health educator. Epstein shared one explanation for the curriculum’s limited attention to birth control. “It is very heteronormative to spend a lot of time talking about just birth control. That is always something that is just in the back of my mind,” Epstein said.
In July of 2022, a friend suggested I listen to a popular podcast called “Binchtopia.” I put on an episode entitled “Popping The Pill” and went for a walk. The episode discussed the history of birth control and the effect the pill has on the human body. Granted, the hosts are not scientists, but it fed a curiosity that had existed since my first Urban Health Class: so many people I know have had mixed experiences with the pill, and so many of them have no idea how it even works, so why don’t we talk about it?
HOW IT WORKS
There are two types of synthetic birth control pills: the combined estrogen and progesterone pill and the progesterone-only pill. Progesterone and estrogen are steroid hormones that regulate the development and function of the uterus.
“Combined hormonal contraception is the most commonly used, and it mostly acts by suppressing ovulation each month, preventing the ovary from releasing an egg,” said Dr. Teresa Safer, member of Pacific Gynecology and Obstetrics Medical Group in an interview with The Urban Legend.
At the beginning of the menstrual cycle, estrogen levels begin to rise. When estrogen reaches peak level at around 14 days, one of the ovaries releases one or more eggs in a process called ovulation. The synthetic hormones in birth control, progesterone and estrogen, block this peak in estrogen levels and prevent the egg from being released. With no egg, there is no possibility of pregnancy.
“[The pill] also has a secondary effect of thickening the cervical mucus, which blocks the sperm from entering the uterus and being able to meet and fertilize an egg,” said Safer.
Besides being 99 percent effective according to the National Health Service, the pill has other benefits and impacts on the body.
“[The pill] regulates your menstrual cycle,” said Rebecca Goldfader, women’s health care nurse practitioner, in an interview with The Urban Legend. “It makes menstrual periods shorter, lighter and less crampy.”
The pill can also reduce the risk of endometrial, ovarian and colorectal cancer according to the National Cancer Institute.
There are many different brands of birth control pills on the market and the effects of them vary. Additionally, each person has a unique reaction to the pill. Some people experience the negative side effects of birth control that doctors warn them about. “Possible side effects are headaches, breast tenderness [and] increase in blood pressure,” said Safer. “Some people notice mood changes.”
However, the common negative side effects are not the only thing to be cautious about when it comes to birth control, there are serious risks with every medication.
“[The pill] can affect your liver and gallbladder,” said Joan Murphy, another women’s health care nurse practitioner, in an interview with The Urban Legend. “If you smoke [while on the pill], you have an increased risk of stroke and heart attack related to clotting.”
“Many people are able to find a good match for them through trialing through several different pills,” said Safer. However, there are some people who don’t find a good match and choose to switch to other contraceptive options. Other common options include the inserted intrauterine device (IUD), which comes in both hormonal and nonhormonal forms, or the birth control patch which you place on your skin like a bandaid and change every 21 days. Every birth control method has its benefits and its drawback so it is important to find the one that works best for you.
EXPERIENCES
While birth control can have a positive impact for some, many people face difficulties while taking the pill, sometimes causing them to go off of it altogether.
“I was put on the pill right when I turned 15 because of period problems and I was on it for about two months before my mom made me stop it,” said Vivienne O’Dell ‘24. “She was like ‘you’re an emotional wreck.’”
O’Dell is not alone. One simple search on a social media platform like TikTok can result in thousands of birth control horror stories that document AFAB people recalling depressive episodes and weight gain, increase in anxiety and stress.
“I’ve seen so many videos being like ‘my body before and after birth control’” said Nora Onek ‘23. “I had been consuming media about weight gain on birth control so I was so hyper-aware of that.”
The birth control pill notoriously affects the way that users see their bodies. “The pill just made me feel awful, like I couldn’t look at myself,” said O’Dell.
Onek took the pill for the first time at age 16 and stopped a year later. “My emotions were hypersensitive, and it felt like I was super anxious and super stressed,” said Onek. “I cried way more on birth control out of stress and frustration that I couldn’t manage my stress the same way I did before.”
This difference in stress response Onek experienced is something scientists have been studying. Research shows that when people start using oral contraception (OC) during puberty/adolescence it can affect how they react to stress. In an article published in the Official Journal of the Society for Behavioral Neuroendocrinology, researchers wrote “our results show that OC use during puberty/adolescence gives rise to a blunted stress response and alters brain activation during working memory processing.” When we are stressed, our bodies release cortisol, which is the primary stress hormone. Cortisol dumps sugar into our bloodstream and preps the body for a flight-or-fight response,essentially regulating our stress response. On the pill, the body can experience a blunted level or absence of cortisol response to stress.
“I have a few friends who got on it recently,” said O’Dell. O’Dell shared the story of her friend who started the pill in December 2022. “She got her period before school got out and she’s still on it [as of December], I’ve heard lots of stories like that.”
Hospitalization is on the more extreme side of what O’Dell shared. “I know people who got on the pill when they were 13 or 14 and they have been hospitalized because they didn’t know about the smoking thing,” said O’Dell, referring to the increased risk for smokers Murphy mentioned earlier.
She shared another example of a friend who took their pill on an empty stomach, something that is not strongly discouraged but advised against. “I know someone who didn’t eat before they took the pill… [they] did that for two days and they were in the hospital for a few days because of it.”
However, these experiences are not universal and should not scare potential consumers away from the pill. “I want to stress that the majority of people I see using the hormonal contraception pill are happy users, it can be a great option for many people,” said Safer.
But for the people like Onek and O’Dell who are not happy users and have experienced a multitude of issues, the shortcomings of the pill can be frustrating.
“Why [is it] whenever a girl has problems with her period or acne, the first thought is a pill that messes with your brain and shoots hormones into your body that you don’t actually need unless you’re using it as a contraceptive?” O’Dell asked.
O’Dell is not the first person to ask this question. Dr. Sarah Hill, author of the best-selling book “This Is Your Brain On Birth Control,” points out how much the pill affects users beyond the intended goal.
“Even though women take the birth control pill for a small number of targeted effects,” said Hill during her TED Talk in 2020, “it has an impact on women’s bodies from head to toe, including the brain.” She goes on to describe how birth control changes people’s levels of sex hormones and therefore changes their brains.
“Our sex hormones are actually a key part of the signaling machinery that our brains uses to create the experience of being the person that we are.”
STARTING THE CONVERSATION
For those who are frustrated, the lack of conversation regarding the pill can be isolating. Hill theorized that the lack of conversation about the negative parts of birth control is due in part to all the good it has done.
Since the pill’s introduction in May of 1950, it has become a cornerstone of feminist politics and helped pave the road to reproductive freedom.
“It is hugely important,” said Epstein. “It gives people with uteruses autonomy and independence in their sexuality and being able to do what they want without consequence.”
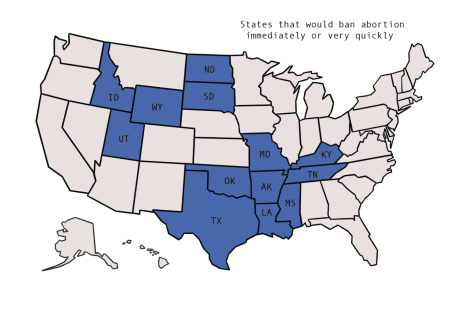
Hill believes this has led people to feel uncomfortable and almost disloyal when they critique the pill. In the context of current politics, with the overturning of Roe v. Wade resulting in a loss of reproductive rights for people across the country, critiquing a widely popular form of contraceptive like the pill can be daunting.
“Talking critically about the pill doesn’t mean that the benefits aren’t going to outweigh the cost,” said Hill in an interview with the Guardian. “It’s not antithetical to women’s rights to talk about this stuff.”
The lack of conversation can also lead to dangerous and impactful misconceptions. For example, issues and stress around perceived weight gain related to the pill. “I was analyzing my weight more than I have before,” said Onek while talking about her time on the pill. “I was so paranoid something was going to happen.”
This anxiety stems from a common myth that birth control can impact your weight. “Research studies do not support weight gain as a side effect,” said Safer. Goldfader seconded this — adding that it can even make some people lose weight. When users do exhibit signs of weight gain it is mostly due to fluid retention — or water weight — not actual weight gain.
The original model of the pill may be a contributing factor in this misconception. When the pill was first created, it had much higher levels of hormones than we use today. Since progesterone can increase appetite and high levels of estrogen can result in water retention, previously weight gain could have been attributed to the pill. The original pill developed in the 1950s contained 150 micrograms (mcg) of estrogen, while today’s typical pill contains around 20 to 50 mcg, according to Official Publication of The College of Family Physicians of Canada. Advances in the pill have addressed weight gain and are no longer of concern.
When Onek went to the doctor to start taking the pill, her doctor did not address this common misconception. “They didn’t say anything about weight gain which made me worry about it more.”
This lack of communication can leave people confused and looking for answers.
“I wasn’t given that much information by my gynecologist and then when I talked to people and looked at social media it seemed like negative things only,” said Onek. “Seeing so much context surrounding the negative effects of birth control might have made me feel like there were more negative effects than there were.”
These miscommunications can be easily addressed by starting nuanced conversations about the way birth control pills impact people. These conversations can, in turn, help people find the form of birth control that works best for them, whether that be the pill or another contraceptive.
For Hill, part of starting the conversation is beginning to find a form of birth control where people don’t have to compromise. “Ideally we want contraception that’s really safe and effective that doesn’t monkey with anyone’s brain,” said Hill in her interview with The Guardian.
This conversation is just beginning, and the answers will not be uniform. Every person has a different experience with birth control and needs different things out of it. The important thing is that we actually just sit down and talk about it.